OCD Test: Obsessive Compulsive Disorder
Table of Contents
A Clinician-Written Self-Reflection Guide Based on Clinical Diagnostic Criteria
By Kelly Pinnick, DBT-Linehan Board of Certification, Certified Clinician | Southside DBT | Telehealth across Georgia
| Important: This guide is a clinician-written educational resource, not a diagnostic tool. Only a licensed mental health professional can diagnose OCD. The self-reflection questions here are designed to help you identify patterns worth discussing with a professional, not to provide a diagnosis. |
There is a particular kind of suffering that OCD produces that most people who have not experienced it do not understand.
It is not about being tidy or liking things organized. It is not about being careful or conscientious. It is not a personality quirk. OCD is the experience of a thought arriving in your mind, often a thought that horrifies or terrifies you, and not being able to make it leave. It is the experience of knowing that the thing you are about to do, checking the stove for the sixth time, washing your hands again, mentally reviewing every conversation for evidence of wrongdoing, will not actually solve anything, and doing it anyway because the alternative is an intolerable level of anxiety.
It is exhausting. It is often deeply shameful. And it is, crucially, treatable.
This guide is written for people who are wondering whether what they are experiencing might be OCD. It covers what OCD actually is, the obsession-compulsion cycle in detail, all twelve major types of OCD with their specific obsessions and compulsions, a clinician-guided self-reflection questionnaire, how OCD is distinguished from similar conditions, how it is diagnosed and treated, and why DBT skills play a meaningful role in OCD treatment for a significant subset of people.
Part 1: What OCD Actually Is
Obsessive Compulsive Disorder is a mental health condition characterized by two defining features that work together in a cycle: obsessions and compulsions.
Obsessions are recurrent, persistent, unwanted thoughts, urges, or images that intrude into consciousness and cause significant distress. The person typically recognizes these thoughts as unwanted and attempts to suppress or neutralize them.
Compulsions are repetitive behaviors or mental acts that the person feels driven to perform in response to an obsession, or according to rigid rules. Compulsions are aimed at reducing distress or preventing a feared outcome, but they provide only temporary relief and in the long term maintain and strengthen the obsession.
Together, obsessions and compulsions create a self-perpetuating cycle that can consume hours of a person’s day and profoundly disrupt functioning, relationships, and quality of life.
What OCD Is Not
OCD is consistently misrepresented in popular culture, and this misrepresentation causes real harm. People whose OCD does not match the cultural stereotype delay seeking help, and people who find the cultural stereotype relatable minimize others’ genuine suffering by applying the label casually.
| What People Think OCD Is | What OCD Actually Is |
| Liking things clean and organized | Intrusive, unwanted thoughts that cause distress regardless of content |
| Being very careful or thorough | Compulsions performed to reduce anxiety, not to achieve results |
| A personality trait or preference | A clinical disorder with neurobiological underpinnings |
| Only about contamination or germs | Present across twelve major subtypes spanning many content areas |
| Something you can stop if you try hard enough | A condition where the harder you try to suppress thoughts, the stronger they become |
| Rare or unusual | Affects approximately 2.2 million adults in the US; one of the most common mental health conditions |
| Kelly’s Perspective | Many clients come to therapy carrying enormous shame about their OCD thoughts, particularly when those thoughts involve harm, sexual content, or morally disturbing imagery. One of the most important things I can offer is this: the presence of a disturbing thought does not reflect your character or your desires. In OCD, the thoughts are ego-dystonic, meaning they feel alien and horrifying precisely because they contradict your values. That contradiction is the disorder, not evidence of who you are. |
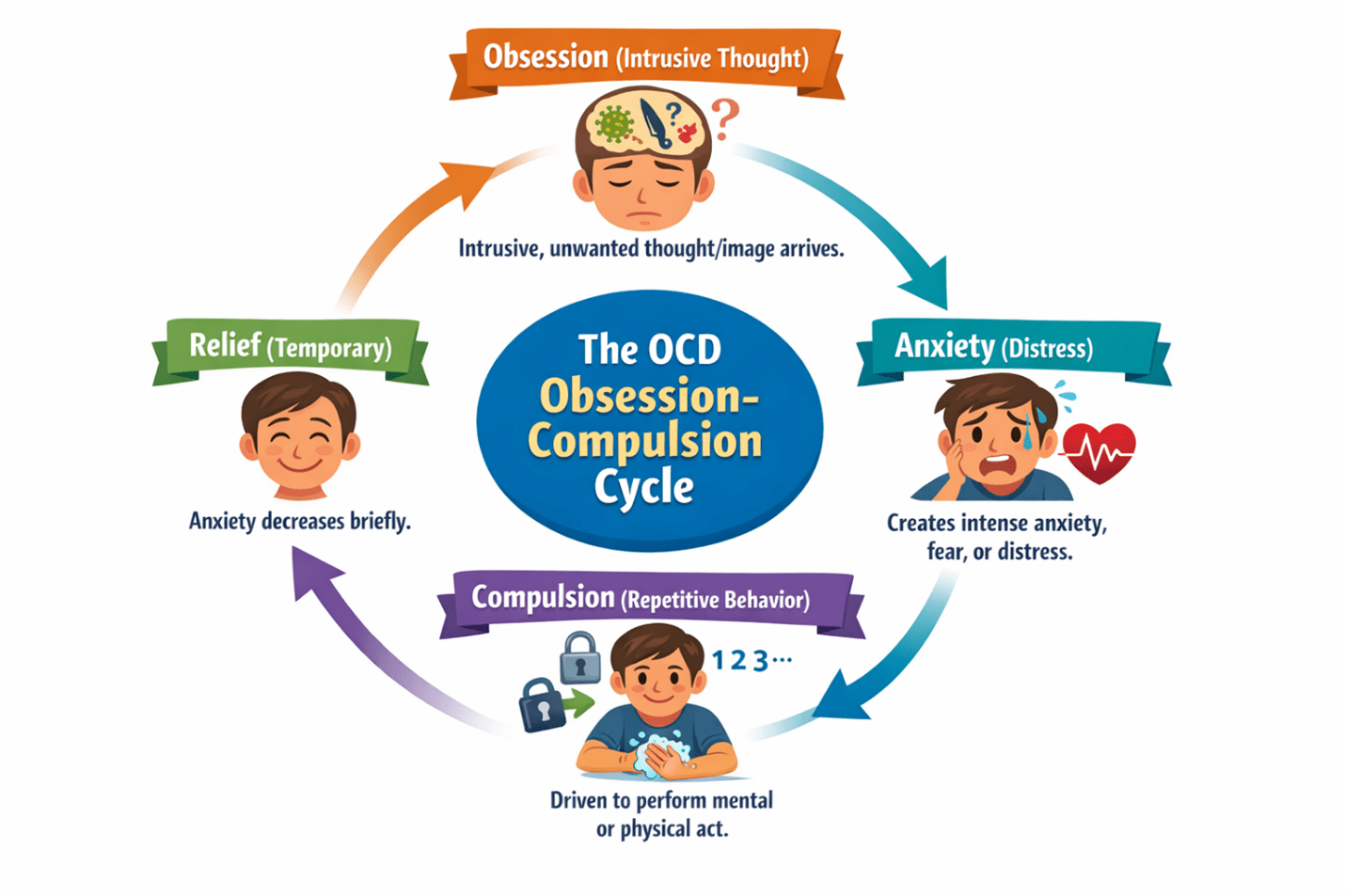
Part 2: The Obsession-Compulsion Cycle — The Engine of OCD
Understanding the cycle that drives OCD is essential both for recognizing it and for understanding why treatment works the way it does.
Step 1: The Intrusive Thought
An intrusive thought, image, or urge enters consciousness. At this point, the thought itself is not yet OCD. Research consistently shows that the vast majority of people, estimated at over ninety percent, experience intrusive thoughts of broadly similar content to OCD obsessions: unwanted thoughts about harm, contamination, taboo sexual content, moral transgression, and uncertainty. The difference is in what happens next.
Step 2: The Appraisal
For a person without OCD, an intrusive thought is registered, noted as uncomfortable or odd, and allowed to pass. For a person with OCD, the thought is appraised as meaningful, dangerous, or personally significant. The cognitive model of OCD, developed by Paul Salkovskis and others, identifies the appraisal of the thought rather than the thought itself as the core mechanism. The OCD sufferer concludes: this thought means something terrible, I am responsible for preventing the feared outcome, and I must act.
Step 3: The Anxiety
The appraisal generates intense anxiety. The anxiety is experienced as unbearable and demands immediate resolution. At this stage, the person is experiencing the full weight of an intrusive thought that they have interpreted as meaningful and threatening.
Step 4: The Compulsion
The compulsion is performed to reduce the anxiety. The reduction is real: the anxiety decreases, temporarily. This temporary relief powerfully reinforces the compulsion through negative reinforcement: the behavior worked, so it will be repeated.
Step 5: The Return
The relief is short-lived. The obsession returns. When it does, the anxiety is often slightly higher than before, because the brain has learned that this thought is a threat requiring action. The threshold for triggering the full cycle gradually lowers. Compulsions become more elaborate and time-consuming. The OCD tightens its grip.
| The compulsion is not the problem. It is the solution that creates the problem. Every compulsion performed teaches the brain that the obsession was a real threat. Treatment works by breaking this reinforcement. |
The Role of Avoidance
Alongside active compulsions, avoidance is a major maintenance mechanism in OCD. People with OCD frequently avoid situations, objects, people, or content that might trigger obsessions. Like compulsions, avoidance provides short-term relief and long-term maintenance of the disorder. The avoided situation is never encountered, so the feared outcome is never disconfirmed, and the belief that avoidance is necessary becomes increasingly entrenched.
Part 3: OCD Self-Reflection Questionnaire
The following questions are adapted from clinical frameworks including the Yale-Brown Obsessive Compulsive Scale. They are not a diagnostic tool and do not produce a clinical score. They are structured reflection prompts designed to help you identify whether your experience aligns with clinically significant OCD patterns.
Answer based on your experience over the past month. Read each question carefully before responding.
| Question 1: Presence of Obsessions |
| Do you experience recurrent, unwanted thoughts, images, or urges that enter your mind even when you do not want them to? |
| The key word is unwanted. OCD obsessions are experienced as intrusive and alien, not as pleasurable rumination or deliberate worry. They arrive without invitation and resist attempts to dismiss them. They may be thoughts about harm, contamination, symmetry, taboo content, doubt, or other themes. If you find yourself thinking things that horrify or disturb you, or that you desperately wish you were not thinking, this is worth exploring. |
| Question 2: Distress and Ego-Dystonicity |
| Do these thoughts cause significant distress, and do they feel inconsistent with who you are or what you believe? |
| Ego-dystonic means the thoughts feel foreign, incompatible with your values, and contrary to your sense of self. This is different from ego-syntonic intrusive thoughts, which feel consistent with the person’s desires, as in certain personality disorders. In OCD, the person is typically horrified by their obsessions precisely because they contradict their values. A person with harm OCD does not want to hurt anyone. That is exactly why the thoughts are so distressing. |
| Question 3: Compulsive Behaviors |
| Do you engage in repetitive behaviors or mental rituals in response to these thoughts, or according to rules that you feel driven to follow? |
| Compulsions can be behavioral: hand washing, checking, arranging, counting, repeating actions. Or they can be mental: reviewing past events, silently praying, mentally neutralizing a thought, seeking internal reassurance. The defining feature is that they are performed in response to obsessions or rigid rules, they are aimed at reducing distress or preventing a feared outcome, and they feel compelled rather than freely chosen. |
| Question 4: Temporary Relief |
| Do the behaviors or rituals reduce your anxiety, but only briefly, with the thoughts or anxiety returning shortly afterward? |
| The temporary nature of the relief is a diagnostic marker. If the compulsion permanently resolved the distress, OCD would be a much less impairing condition. The temporary relief is what makes the cycle so difficult to break: the compulsion works just enough, and just briefly enough, to keep the person coming back to it while the underlying cycle strengthens. |
| Question 5: Time and Impairment |
| Do obsessions and compulsions consume a significant amount of your time, more than an hour per day on average, or do they significantly interfere with your daily functioning, relationships, or work? |
| The one-hour threshold is the clinical benchmark from the DSM-5. Many people with OCD far exceed this. The time includes both the direct performance of compulsions and the time spent in anticipatory anxiety, avoidance, and mental rituals. Impairment can look like being late to work because you cannot leave the house until compulsions are completed, avoiding relationships because of relationship OCD, or being unable to sleep because of intrusive thoughts. |
| Question 6: Recognition of Excessiveness |
| Do you recognize, at least some of the time, that your obsessions or compulsions are excessive or unreasonable, even while feeling unable to stop them? |
| The DSM-5 notes that insight in OCD exists on a spectrum from good insight to absent insight. Most people with OCD have some awareness that their fears are excessive or irrational, and yet this recognition does not reduce the anxiety or the compulsive urge. This is one of the most frustrating aspects of OCD: knowing that the thought is not rational does not make it less distressing. |
| Question 7: Avoidance |
| Do you avoid certain situations, places, people, objects, or activities to prevent triggering your obsessions? |
| Avoidance in OCD is often underrecognized because it looks like ordinary caution or preference rather than a symptom. Someone with contamination OCD may decline social invitations because they cannot control the hygiene of others’ homes. Someone with harm OCD may avoid being around children. Someone with checking OCD may avoid any situation where they might need to be responsible for locking up. The avoidance progressively narrows life without the person necessarily recognizing it as part of OCD. |
| Question 8: Reassurance Seeking |
| Do you frequently seek reassurance from others, or repeatedly check information online or elsewhere, to manage OCD-related anxiety? |
| Reassurance seeking is a compulsion that operates through other people or information sources. Asking a partner repeatedly whether something terrible happened, googling symptoms obsessively, or calling a family member to confirm safety are all reassurance-seeking behaviors. Like other compulsions, reassurance provides temporary relief and long-term maintenance of the obsessive cycle. Reassurance seeking is also particularly relevant to relationship OCD and health anxiety presentations. |
| Question 9: Duration and Persistence |
| Have these experiences been present for at least several weeks, and are they relatively consistent rather than tied only to a specific stressful event? |
| OCD is a persistent condition, not a temporary stress response. While stressors can exacerbate OCD, the condition itself does not resolve when the stressor resolves. Temporary intrusive thoughts that arise during acute stress and then fully remit may reflect normal stress responses rather than OCD. The persistence and independence from specific stressors is clinically important. |
Understanding Your Responses
| Number of Questions That Apply | What This May Suggest |
| 1 to 2 questions, mildly | May reflect normal intrusive thoughts or situational stress. Monitor and discuss with a professional if distress continues. |
| 3 to 4 questions consistently | Possible subclinical OCD or anxiety-related pattern worth professional evaluation. Significant distress warrants assessment. |
| 5 or more questions, ongoing | Pattern is consistent with clinically significant OCD. Professional evaluation and evidence-based treatment is strongly recommended. |
Part 4: Twelve Types of OCD — Explained in Full
OCD presents differently across individuals. The content of obsessions and the nature of compulsions vary enormously. Understanding the specific presentation matters because different types can look very different, and some subtypes carry particularly heavy shame burdens that delay help-seeking.
| Contamination OCD |
| Common Obsessions: Fear of germs, illness, bodily fluids, chemicals, environmental toxins, or moral contamination from people or objects. Common Compulsions: Excessive hand washing, showering, cleaning. Avoiding touching surfaces, door handles, other people. Decontamination rituals. |
| Clinical Note: The most commonly depicted type of OCD in popular culture. Contamination fears can be physical or moral: the sense of being contaminated by a person or situation rather than a physical substance. |
| Checking OCD |
| Common Obsessions: Intrusive doubts about whether something harmful will happen because of something undone: fire, flooding, break-ins, accidents. Common Compulsions: Repeatedly checking locks, appliances, lights, documents. Mentally reviewing actions. Asking others to confirm. Taking photos as proof. |
| Clinical Note: Checking compulsions are sustained by doubt: no amount of checking fully eliminates the uncertainty. The more checking occurs, the less reliable memory becomes, which increases doubt further. |
| Symmetry and Order OCD |
| Common Obsessions: Intrusive discomfort with asymmetry, incompleteness, or items not in the right place. Often accompanied by a felt sense that something is not right. Common Compulsions: Arranging and rearranging objects. Repeating actions until they feel right. Counting. Balancing symmetrical actions. |
| Clinical Note: This type often involves the Just Right phenomenon: an internal sense of wrongness that persists until the compulsion achieves a feeling of rightness. It is driven by sensory discomfort rather than feared consequences in many cases. |
| Harm OCD |
| Common Obsessions: Intrusive thoughts, images, or urges about causing harm to oneself or others, including violent imagery. The person does not want to act on these thoughts. Common Compulsions: Avoiding potential weapons or sharp objects. Avoiding being around vulnerable people. Mental reviewing for evidence of having harmed. Seeking reassurance. Confessing. |
| Clinical Note: Harm OCD is often among the most distressing types because the content of the thoughts is so contrary to the person’s values. The presence of harm thoughts in OCD is not evidence of violent intent. People with harm OCD typically have extremely strong aversions to violence. |
| Pure O (Primarily Obsessional OCD) |
| Common Obsessions: Intrusive thoughts, images, or urges across various content areas where the compulsions are primarily mental rather than behavioral and therefore invisible to others. Common Compulsions: Mental reviewing and analysis of the thought. Mental neutralizing. Internal reassurance rituals. Thought suppression attempts. |
| Clinical Note: Pure O is a misnomer: there are always compulsions, but they are covert mental acts rather than visible behaviors. Pure O is significantly underdiagnosed because sufferers and clinicians may not recognize the mental compulsions as compulsions. |
| Relationship OCD (ROCD) |
| Common Obsessions: Intrusive doubts about the rightness of a relationship, whether one truly loves their partner, whether the partner is right for them, or intrusive thoughts about perceived flaws in the partner. Common Compulsions: Mentally reviewing feelings about the partner. Comparing the relationship to others. Testing feelings by imagining breakup scenarios. Seeking reassurance about love. |
| Clinical Note: ROCD causes profound suffering and frequently destabilizes genuine relationships. The presence of doubt in ROCD is a symptom of OCD, not evidence that the relationship is wrong. Partners of people with ROCD also require support. |
| Scrupulosity OCD (Religious and Moral OCD) |
| Common Obsessions: Intrusive thoughts about having sinned, offended God, violated moral codes, or having done something unforgivable. May involve blasphemous intrusive thoughts. Common Compulsions: Excessive prayer, confession, or seeking forgiveness. Mentally reviewing actions for moral transgressions. Avoidance of religious contexts that trigger thoughts. |
| Clinical Note: Scrupulosity OCD is particularly prominent in communities with strong religious or moral frameworks. It is often misidentified as excessive religiosity or genuine guilt rather than OCD. Religious leaders who understand OCD can be valuable allies in treatment. |
| Health Anxiety OCD |
| Common Obsessions: Intrusive fears about having a serious illness or having missed a symptom. Persistent concern that symptoms indicate cancer, neurological conditions, or other severe disease. Common Compulsions: Repeatedly checking body for symptoms. Repeated medical appointments. Compulsive online health research. Seeking reassurance from doctors or family. |
| Clinical Note: Health anxiety OCD overlaps significantly with somatic symptom disorder and illness anxiety disorder. The distinguishing feature in OCD is the obsessive-compulsive cycle rather than generalized health worry. |
| Sexual Orientation OCD (SO-OCD) |
| Common Obsessions: Intrusive doubts about one’s sexual orientation, not reflecting actual uncertainty about identity. Distressing to the person, who typically finds the doubt alien and unwanted. Common Compulsions: Mentally testing attraction responses. Compulsive checking of reactions to others. Reviewing past behavior for evidence. Seeking reassurance. |
| Clinical Note: SO-OCD is not the same as genuine questioning of sexual orientation. People with SO-OCD are typically not uncertain about their identity in a ways that feels authentic: the doubt feels imposed and unwanted. Clinicians unfamiliar with OCD may misidentify this as orientation confusion. |
| Pedophilia OCD (POCD) |
| Common Obsessions: Intrusive thoughts, images, or urges of a sexual nature involving children. The person is horrified by these thoughts and has no desire to act on them. Common Compulsions: Avoidance of children and situations involving children. Compulsive mental reviewing for evidence of attraction. Seeking reassurance. Confessing. |
| Clinical Note: POCD is one of the most stigmatized and under-discussed OCD presentations. It is critical to understand that intrusive thoughts in OCD are ego-dystonic: they are horrifying precisely because they contradict the person’s values and desires. People with POCD are not predators. They are suffering. Evidence-based treatment is effective. |
| Hoarding OCD |
| Common Obsessions: Fear of discarding items that might be needed, or intrusive sense that discarded items will cause harm or loss. Different from hoarding disorder but can co-occur. Common Compulsions: Inability to discard items. Excessive acquisition. Mental reviewing of every item before potential disposal. |
| Clinical Note: Hoarding OCD is distinct from hoarding disorder, though both involve difficulty with discarding. In OCD, the difficulty is driven by obsessional fears rather than the emotional attachment and perceived utility that characterizes hoarding disorder. |
| Existential OCD |
| Common Obsessions: Intrusive questions about the nature of reality, existence, consciousness, meaning, or identity. Questions such as: How do I know I am real? What is the point of anything? Am I the same person I was yesterday? Common Compulsions: Compulsive philosophical analysis. Seeking reassurance that reality is real. Mental reviewing of existential questions without resolution. |
| Clinical Note: Existential OCD is often dismissed as philosophical curiosity rather than recognized as OCD. The defining feature is that the questions produce significant distress and the person cannot tolerate the uncertainty, rather than finding philosophical exploration interesting or enjoyable. |
Part 5: OCD vs Other Conditions — The Most Common Confusions
OCD overlaps symptomatically with several other conditions, and misdiagnosis is common. Understanding the distinctions matters because the treatments are different.
OCD vs Generalized Anxiety Disorder
Both conditions involve persistent worry. The key distinction is the nature of the worry and the response to it. GAD involves worry about realistic, everyday concerns that fluctuates naturally. OCD involves specific obsessional content that triggers compulsions, and the worry is characterized by intrusive, ego-dystonic quality rather than ordinary rumination. The presence of ritualistic compulsions points toward OCD rather than GAD.
OCD vs OCPD (Obsessive Compulsive Personality Disorder)
These conditions are frequently confused due to similar names. OCPD is a personality disorder characterized by perfectionism, rigidity, control, and preoccupation with orderliness that the person finds ego-syntonic: they believe their way of doing things is correct and appropriate. OCD involves ego-dystonic intrusive thoughts that the person wishes they were not having. A person with OCPD does not experience their orderliness as a problem. A person with OCD does.
OCD vs Depression with Rumination
Depression involves persistent negative rumination about the past, self-worth, and the future. This rumination is negative but does not typically have the intrusive, alien quality of OCD obsessions, and it is not followed by specific compulsive rituals. OCD and depression frequently co-occur, with depression developing secondary to the suffering caused by OCD. Both may require treatment.
OCD vs Psychosis
People with OCD sometimes fear they are going crazy, but OCD is not a psychotic condition. People with OCD maintain reality testing: they recognize, at least some of the time, that their fears are excessive. In psychosis, the person typically does not recognize their beliefs as unusual or inconsistent with reality. OCD with poor insight can be misidentified as psychosis, but they are distinct conditions requiring different treatments.
OCD vs Body Dysmorphic Disorder
Body dysmorphic disorder involves obsessive preoccupation with a perceived defect in physical appearance and is classified in the DSM-5 as an OCD-related disorder. The compulsions in BDD are specifically aimed at checking, concealing, or fixing the perceived flaw. BDD and OCD can co-occur and share significant neurobiological overlap, but they are distinct in their content focus.
Part 6: How OCD Is Diagnosed
OCD is diagnosed by a licensed mental health professional through clinical interview. There is no blood test, brain scan, or questionnaire that can diagnose OCD. The Yale-Brown Obsessive Compulsive Scale, or Y-BOCS, is the most widely used standardized assessment tool in OCD evaluation, but it is used to assess severity once OCD is identified rather than as a standalone diagnostic instrument.
The Diagnostic Criteria
The DSM-5 requires the following for an OCD diagnosis:
- Presence of obsessions, compulsions, or both
- Obsessions and compulsions are time-consuming, taking more than one hour per day, or cause clinically significant distress or impairment in social, occupational, or other important areas of functioning
- Symptoms are not attributable to the physiological effects of a substance or another medical condition
- The disturbance is not better explained by another mental disorder
The clinician also specifies the level of insight: good or fair insight, poor insight, or absent insight. This specification matters because it affects treatment planning and prognosis.
Why OCD Is Frequently Missed or Misdiagnosed
OCD goes undiagnosed for an average of 14 to 17 years from symptom onset in many cases. This extraordinary delay has several causes.
- Shame: The content of OCD obsessions, particularly harm, sexual, and scrupulosity subtypes, is so shameful that many people cannot bring themselves to disclose it to a clinician. They describe anxiety without revealing the specific thoughts driving it.
- Clinician unfamiliarity: Mental health providers who are not trained in OCD recognition may miss covert compulsions, misidentify OCD presentations as anxiety disorders or depression, or fail to ask about OCD-specific content.
- Reassurance-based treatment: Clinicians who primarily offer reassurance to OCD patients inadvertently function as a reassurance compulsion, maintaining rather than treating the disorder.
- Pure O presentations: When compulsions are mental rather than behavioral, neither the person nor the clinician may recognize them as compulsions.
- Cultural and religious context: Scrupulosity and other OCD presentations that intersect with cultural or religious practice may be misidentified as normal expressions of faith or culture rather than OCD.
Part 7: Evidence-Based Treatment for OCD
OCD is one of the most treatable mental health conditions when approached with the right methods. Two interventions have the strongest evidence base and should be considered first-line treatment.
Exposure and Response Prevention (ERP)
ERP is the gold standard psychological treatment for OCD and has the most robust evidence base of any psychological intervention for any specific mental health condition. It is a form of Cognitive Behavioral Therapy specifically designed for OCD.
ERP works by systematically exposing the person to the situations, thoughts, or stimuli that trigger obsessions, while preventing the performance of compulsions. This breaks the reinforcement cycle described in Part 2.
The mechanism is habituation and inhibitory learning: the person learns, through direct experience, that the feared outcome does not occur, that the anxiety diminishes without compulsions being performed, and that the intrusive thought loses its power when it is not reinforced through compulsive responding.
ERP is not comfortable. It requires deliberately inducing anxiety and tolerating it without compulsive relief. This is the mechanism of change. A skilled ERP therapist constructs a graduated hierarchy of exposures and guides the client through the process with clinical expertise.
What ERP Looks Like in Practice
ERP begins with psychoeducation about the obsession-compulsion cycle and the rationale for exposure. The therapist and client then build an exposure hierarchy: a list of feared situations ranked from least to most anxiety-provoking. The client begins with lower-level exposures and progressively works up the hierarchy.
For contamination OCD, an exposure might involve touching a doorknob and then delaying hand washing for progressively longer periods until the compulsion is resisted entirely. For checking OCD, it might involve locking the door and driving away without returning to check.
For mental obsessions in Pure O, ERP takes the form of imaginal exposure: deliberately thinking the obsessional thought without performing mental neutralizing rituals, allowing the anxiety to rise and then naturally subside.
Medication for OCD
The medications with the strongest evidence for OCD are serotonin reuptake inhibitors. The following are FDA-approved for OCD:
- Fluvoxamine (Luvox): First SSRI specifically approved for OCD
- Sertraline (Zoloft): Commonly used due to favorable tolerability profile
- Paroxetine (Paxil): Effective but higher rate of discontinuation effects
- Fluoxetine (Prozac): Frequently used, particularly with children
- Clomipramine (Anafranil): A tricyclic antidepressant with strong OCD evidence; typically used when SSRIs have been insufficient
OCD typically requires higher doses of SSRIs than depression, and the response time is longer, often eight to twelve weeks. Combination of medication and ERP consistently produces better outcomes than either treatment alone.
Intensive OCD Treatment
For severe or treatment-resistant OCD, intensive outpatient programs offering multiple hours of ERP per week have strong evidence. Residential treatment is available for the most severe presentations. Deep brain stimulation has been approved for treatment-resistant OCD in specific cases. The key principle is that the same mechanisms apply at any intensity: disrupting the obsession-compulsion cycle through exposure and response prevention.
Part 8: OCD and Emotion Dysregulation — Where DBT Skills Are Relevant
DBT was not developed for OCD and is not a first-line treatment for OCD in the way ERP is. However, DBT skills play a meaningful role for a significant subset of people with OCD, and understanding when and how they are relevant is clinically important.
When DBT Skills Are Particularly Relevant in OCD
DBT distress tolerance skills are directly relevant to the experience of sitting with obsessional anxiety without performing compulsions. ERP requires the person to tolerate high levels of anxiety without the relief of compulsions. For people whose emotional regulatory capacity is limited, this is extremely difficult. DBT distress tolerance skills, particularly the TIPP skills and radical acceptance, provide a framework for tolerating that distress while the habituation process does its work.
Mindfulness skills from DBT also directly support ERP. Mindful observation of obsessional thoughts, without judgment and without compulsive responding, is precisely the stance that ERP requires. The DBT skill of observing thoughts as thoughts rather than facts, noticing them without fusing with them, directly supports the defusion that ERP aims to produce.
For people with OCD who also have co-occurring BPD, significant trauma, or severe emotional dysregulation, DBT Stage 1 skills may be needed before intensive ERP can be effectively engaged. Attempting high-intensity exposure work without adequate emotional regulatory capacity can produce flooding rather than habituation.
| Clinical Integration | In practice, the most effective approach for OCD with co-occurring emotion dysregulation involves DBT skills training for stabilization alongside graduated ERP. The DBT skills provide the window of tolerance within which the ERP can produce its effects. This is not diluted ERP. It is sequenced and scaffolded treatment that meets the client where their regulatory capacity actually is. |
Part 9: Recovery from OCD — What the Evidence Shows
OCD is a chronic condition in many cases, but chronic does not mean untreatable or unchanging. The research on treatment outcomes for OCD is genuinely encouraging.
Meta-analyses of ERP for OCD consistently find large effect sizes, with clinically significant symptom reduction in sixty to eighty percent of people who complete treatment. Combination of ERP and medication produces the highest response rates. Intensive treatment programs produce faster and often deeper initial results.
Relapse is possible, particularly under stress or without maintenance practice. However, people who have learned ERP skills have the tools to address relapse when it occurs. Many people with OCD describe periods of near-complete symptom remission. Others manage OCD to the point where it no longer significantly interferes with their lives even when some symptoms remain.
What Recovery Looks Like
Recovery from OCD is not the elimination of all intrusive thoughts. Intrusive thoughts are a universal human experience. Recovery means that intrusive thoughts no longer derail your life. It means being able to have an unwanted thought and let it pass without compulsive responding. It means your anxiety about the thought is tolerable rather than unbearable. It means OCD is no longer determining your choices.
Many people who have recovered from severe OCD describe the experience of ERP as one of the hardest and most transformative things they have ever done. The willingness to feel the anxiety without escaping it changes the relationship to fear in ways that extend far beyond OCD symptoms.
When to Seek Professional Help
If your self-reflection through this guide has left you recognizing patterns that align with OCD, the most important step you can take is to reach out to a mental health professional with specific training in OCD and ERP.
Not all therapists are trained in ERP. It is appropriate to ask directly whether a potential therapist is trained in ERP for OCD, how many OCD clients they have treated, and what their treatment approach involves. The International OCD Foundation maintains a provider directory of ERP-trained clinicians.
The shame that OCD produces, particularly around its content, is not a reason to delay seeking help. It is a reason to find a clinician who understands OCD well enough to hold that content without judgment, which all well-trained OCD clinicians do.
OCD is treatable. The cycle that feels inescapable can be interrupted. The thoughts that feel permanent can lose their power. The life that OCD has narrowed can be recovered.
| Struggling with OCD or Anxiety-Related Symptoms? Southside DBT provides evidence-based treatment for anxiety, OCD-related emotion dysregulation, and co-occurring conditions including BPD and PTSD via telehealth across Georgia. Kelly Pinnick | DBT-Linehan Board of Certification, Certified Clinician (770) 880-2538 | kelly@southsidedbt.com Accepting: Aetna | Anthem BCBS GA | Cigna | United Healthcare | Self-Pay $150/session |
Crisis Resources: 988 Suicide and Crisis Lifeline: Call or Text 988 | Crisis Text Line: Text HELLO to 741741
