What Is Emotional Dysregulation?
Table of Contents
A Comprehensive Guide to Causes, Signs, the Neuroscience, and DBT-Based Treatment
By Kelly Pinnick, DBT-Linehan Board of Certification, Certified Clinician | Southside DBT | Telehealth across Georgia
Everyone has had the experience of a feeling that arrived too fast, too intensely, and produced a reaction that the calmer version of you later regretted. A sharp word that did not need to be sharp. A tearful breakdown over something that was not actually catastrophic. A surge of rage that lasted ten minutes and left you exhausted and confused.
For most people, these moments are exceptions. For people with emotional dysregulation, they are the pattern.
Emotional dysregulation is not about being weak, dramatic, or immature. It is about having an emotional system that responds with greater intensity, less predictability, and slower return to baseline than what most people experience. It is one of the most pervasive, most impairing, and most frequently misunderstood features of a wide range of mental health conditions, from BPD and PTSD to ADHD, depression, and anxiety.
This guide goes substantially further than Cleveland Clinic’s overview of the topic. It covers the neuroscience of why emotional dysregulation happens, the biosocial theory that best explains how it develops, what it actually looks like in daily life with real-world examples, how to distinguish it from being sensitive or reactive, the specific conditions it is associated with, and most importantly, how DBT directly addresses it with specific, evidence-based skills.
What Emotional Dysregulation Is — and What It Is Not
Emotional dysregulation refers to difficulty managing the intensity, duration, and expression of emotional responses in ways that are appropriate to the situation and consistent with longer-term goals and values.
Emotion regulation is not the suppression of emotion. It is not the ability to never feel intensely or to appear unbothered. It is the capacity to feel emotions, experience their full content, and direct behavioral responses in ways that are not driven purely by the emotion’s immediate demand. Regulation means you can be angry without destroying something. You can be terrified without fleeing. You can be devastated without being paralyzed.
Emotional dysregulation is the impairment of this capacity. It exists on a spectrum: from occasional difficulty managing strong emotions under stress, which is universal, to pervasive, daily emotional experiences that feel overwhelming, unpredictable, and impossible to control.
The Key Dimensions of Emotional Dysregulation
Researchers have identified several distinct dimensions that together constitute emotional dysregulation. Understanding these dimensions is more clinically useful than a single definition.
| Dimension | What It Means | What It Looks Like |
| Emotional sensitivity | Lower threshold for emotional activation | Getting upset in situations others find mildly annoying or neutral |
| Emotional reactivity | More intense response once emotion is activated | Feeling devastated when others feel disappointed; furious when others feel annoyed |
| Slow return to baseline | Longer time to recover from emotional activation | Still feeling the emotion hours or days after the triggering event has passed |
| Difficulty identifying emotions | Inability to accurately label what is being felt | Knowing something is wrong but not knowing whether it is anger, grief, shame, or fear |
| Avoidance of emotional experience | Suppression or escape from difficult emotions | Substance use, self-harm, dissociation, or excessive distraction to avoid feeling |
| Impulsive responding | Acting on emotion before reflection is possible | Sending a message you regret, walking out, saying something hurtful |
| Limited access to regulation strategies | Not knowing what to do when overwhelmed | Feeling helpless or out of control when emotions are intense |
The Neuroscience of Emotional Dysregulation
Cleveland Clinic’s article says that emotional dysregulation happens when parts of the brain do not talk or work together as they should. That is technically accurate and entirely unhelpful. Here is what is actually happening.
The Amygdala and the Threat Response
The amygdala is the brain’s threat detection center. It receives sensory information faster than the prefrontal cortex can analyze it, and it fires a threat response before conscious thought has had time to evaluate whether a genuine threat exists. In the context of emotion, the amygdala is responsible for the rapid escalation of emotional responses to perceived threats, social rejection, loss, or danger.
In people with emotional dysregulation, the amygdala appears to have a lower activation threshold: it fires in response to stimuli that do not trigger the same response in others, and when it does fire, it does so with greater intensity. This is not a character defect. It is a neurological difference that has both genetic and developmental origins.
The Prefrontal Cortex and Top-Down Regulation
The prefrontal cortex is responsible for what researchers call top-down regulation: the capacity to modulate, redirect, and contextualize emotional responses generated by subcortical structures. When the prefrontal cortex is functioning effectively, it receives the amygdala’s threat signal and evaluates it: is this actually dangerous? What is the appropriate response? What are the consequences of acting on this feeling?
In emotional dysregulation, this top-down regulation is impaired. The prefrontal cortex does not effectively modulate the amygdala’s response. There are several reasons this can happen: developmental factors that affected the prefrontal cortex’s maturation, chronic stress that chronically dysregulates the system, trauma that has sensitized the threat response, and the sheer intensity of the emotion itself, which at very high levels floods the prefrontal cortex and reduces its capacity to function.
The Role of the Autonomic Nervous System
The autonomic nervous system plays a direct role in emotional dysregulation through its two branches: the sympathetic system, which activates the fight-or-flight response, and the parasympathetic system, which promotes rest and recovery. In people with emotional dysregulation, the sympathetic system activates more easily and more intensely, and the parasympathetic system takes longer to re-engage. The result is a nervous system that is frequently in a state of elevated arousal and slow to return to baseline.
This is why the physical symptoms of emotional dysregulation, racing heart, muscle tension, shallow breathing, flushing, are so prominent. These are not metaphors for strong emotion. They are the direct physiological expression of autonomic activation.
Neuroplasticity and the Possibility of Change
Here is what makes emotional dysregulation genuinely treatable rather than merely manageable: the brain is neuroplastic, meaning it changes in response to experience. The neural pathways that underlie emotional dysregulation, sensitized amygdala responses, weak prefrontal inhibition, poorly integrated autonomic regulation, can be remodeled through consistent, repeated practice of regulatory behaviors.
This is exactly what DBT targets. Each time a DBT skill is used in a high-distress moment, it practices and strengthens the prefrontal pathways that modulate the amygdala response. Regulation is literally a skill that is built in the brain through use.
| Emotional dysregulation is not a permanent neurological state. The brain changes in response to what it practices. Every time a regulation skill is used effectively, it strengthens the neural circuits that make regulation possible in the future. |
The Biosocial Theory — How Emotional Dysregulation Develops
Marsha Linehan, who developed DBT specifically to treat the severe emotional dysregulation associated with BPD, proposed the biosocial theory as the most comprehensive explanation for how emotional dysregulation develops and persists. This theory is one of the most clinically useful frameworks in all of mental health.
The Biological Component
The biosocial theory begins with biology. Some individuals are born with a nervous system that is more emotionally sensitive and reactive than others. This heightened sensitivity is not a pathology in itself. It is a variation in biological temperament that has genetic components and that is present from birth.
Children who are biologically more emotionally sensitive feel emotions more intensely, react more quickly, and return to baseline more slowly than less sensitive children. Under the right conditions, this sensitivity can become a strength: deeper empathy, richer emotional experience, greater attunement to others. Under the wrong conditions, it becomes the basis for severe dysfunction.
The Social Component: The Invalidating Environment
The biosocial theory proposes that emotional dysregulation develops at the intersection of biological sensitivity and what Linehan calls an invalidating environment: a relational context in which the child’s emotional experiences are consistently dismissed, minimized, criticized, or punished.
An invalidating environment communicates: your feelings are wrong, excessive, inappropriate, attention-seeking, or simply not acceptable. The messages can be explicit: stop crying or I’ll give you something to cry about. Or they can be subtle: recurring dismissal, changing the subject when emotion is expressed, or an atmosphere in which emotional expression was simply never modeled or welcomed.
The combination of high biological sensitivity and invalidating environment is particularly damaging because the child who needs the most help learning to identify and manage emotions receives the least. The sensitive child who needs attunement gets dismissal. The result is an emotional system that developed without adequate scaffolding: one that generates intense responses but has not learned to process or manage them.
What the Biosocial Theory Changes
The biosocial theory changes the clinical conversation in one essential way: it locates the origin of emotional dysregulation in a transaction between biology and environment, not in personal failure or moral weakness.
People with severe emotional dysregulation have almost universally been told, explicitly or implicitly, that they are too much, too sensitive, overreacting, or dramatic. The biosocial theory contextualizes these experiences: they are not character flaws. They are the predictable result of a sensitive nervous system that did not receive the developmental support it needed. This is not exculpatory. It is explanatory. And the distinction matters enormously for treatment engagement.
| Kelly’s Perspective | When I explain the biosocial theory to clients, I consistently see something shift. The shame about being this way begins to loosen. Not because they no longer have to do the work of change, but because they understand for the first time that the way they are makes sense. That is not a small thing. It is often the beginning of genuine therapeutic engagement. |
The Emotional Dysregulation Spectrum — Flooding and Shutdown
Emotional dysregulation does not look the same in every person or in every moment. It exists on a spectrum with two characteristic extremes that DBT specifically addresses.
Emotional Flooding
Flooding is the state of being overwhelmed by emotional intensity. When flooding occurs, the prefrontal cortex is effectively offline, and behavior is driven almost entirely by the emotional system. The person may say or do things that do not align with their values or their calmer judgment. They may feel out of control, unable to stop themselves, or as though they are watching themselves from the outside.
Flooding can manifest as rage, panic, overwhelming grief, or shame spirals. It is characterized by high physiological arousal, rapid escalation, and behavioral responses that prioritize immediate emotional relief over long-term consequences.
Emotional Shutdown
Shutdown is the opposite pole: the state of emotional numbness, dissociation, or withdrawal that occurs when emotional intensity has exceeded the system’s capacity to process it. The person becomes flat, checked out, unable to feel or respond.
Shutdown is often mistaken for calmness or indifference. It is neither. It is the nervous system’s emergency brake: a freeze response to emotional overwhelm. People in shutdown may appear fine while experiencing profound internal distress or inaccessibility. They may respond to questions with I don’t know or feel nothing while being in the middle of an emotionally significant situation.
The Oscillation Between States
Many people with significant emotional dysregulation oscillate between flooding and shutdown, sometimes within the same day. An intense emotional episode produces flooding. The flooding exhausts the system, which then collapses into shutdown. The shutdown is then punctuated by another flooding episode as suppressed emotions break through.
This oscillation is one of the most confusing and demoralizing features of emotional dysregulation. The person, and often the people around them, cannot predict which state they will be in or why the transition happens. DBT’s window of tolerance concept provides a framework for understanding this.
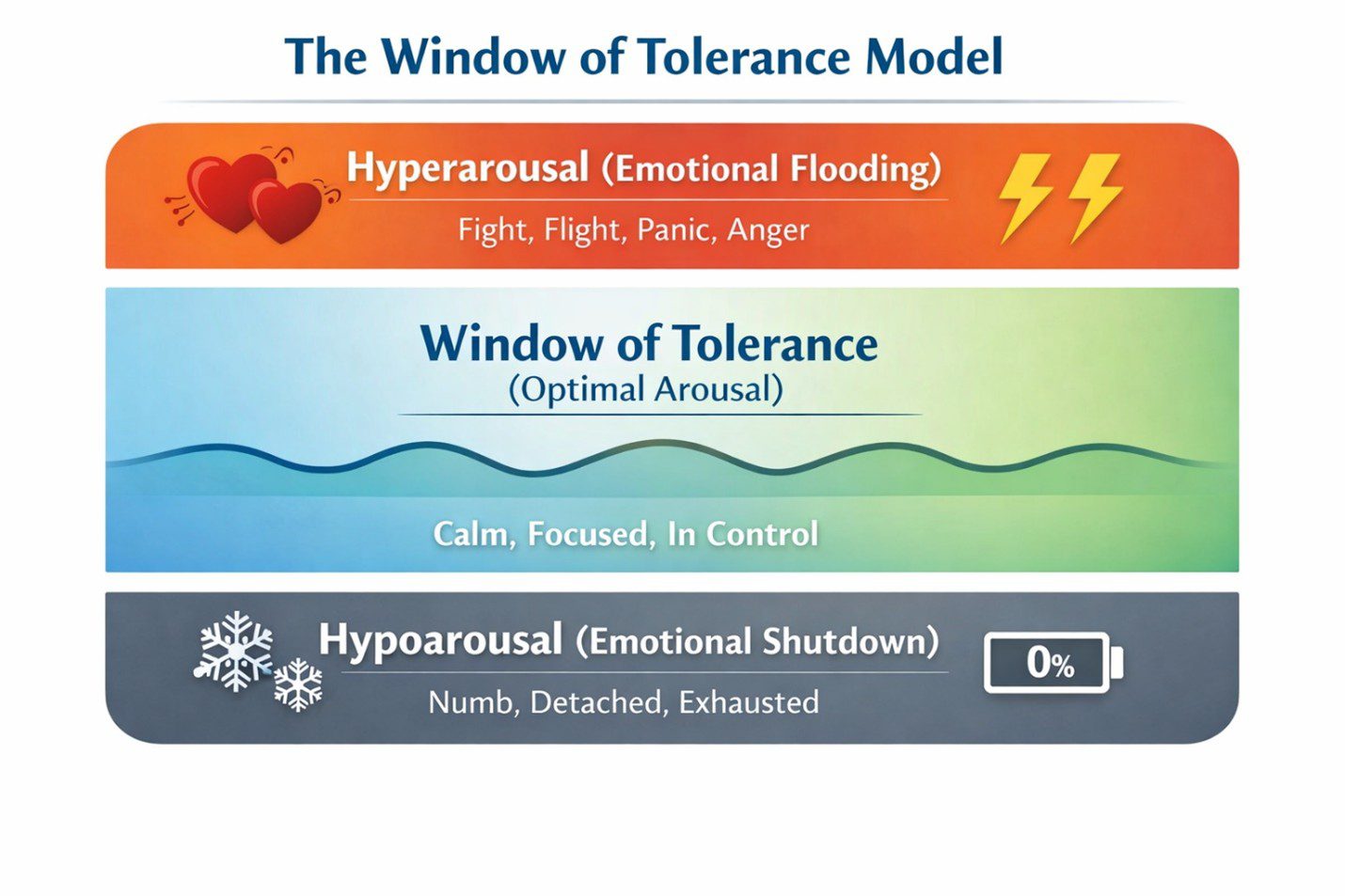
The Window of Tolerance
The window of tolerance, a concept developed by Dan Siegel and integrated into DBT and trauma treatment, describes the zone of optimal emotional arousal in which a person can think clearly, feel their emotions, and respond flexibly. Above the window is hyperarousal, flooding. Below it is hypoarousal, shutdown.
People with emotional dysregulation have a narrower window of tolerance than others, meaning they leave the window more easily, stay outside it longer, and find it harder to return. The goal of DBT treatment is not to eliminate strong emotions but to widen the window: to build the regulatory capacity that allows more emotional experience to be processed within a manageable range.
What Emotional Dysregulation Actually Looks Like in Daily Life
Clinical descriptions of emotional dysregulation are easy to misread as distant or abstract. Here are concrete real-world scenarios that illustrate what emotional dysregulation looks and feels like from the inside and outside.
| Scenario 1: Work Feedback |
| What It Looks Like From Outside: The person becomes visibly upset, defends themselves intensely, and is distracted for the rest of the day. Colleagues notice they seem to have taken it very hard. What Is Actually Happening: The feedback activated a deep shame response: I am failing, I am not good enough. The amygdala fired as though the job itself was at stake. The prefrontal cortex could not modulate the response fast enough. What felt proportionate from the inside was not proportionate to the external situation. |
| The Situation: A manager gives mild, constructive feedback on a presentation. The feedback is genuinely minor. |
| Scenario 2: Unanswered Text Message |
| What It Looks Like From Outside: The person becomes increasingly anxious, then hurt, then angry. They may send follow-up messages, which they later regret. They feel the silence as rejection. What Is Actually Happening: The silence activated a fear of abandonment that is neurologically processed as a genuine threat. The waiting period produced real, physical anxiety. This is not irrationality. It is a sensitized threat-detection system responding to ambiguity with its maximal interpretation. |
| The Situation: A friend does not reply to a text for several hours. No conversation has indicated any problem. |
| Scenario 3: An Argument |
| What It Looks Like From Outside: The conversation escalates rapidly. One person is shouting. The other has gone completely silent. The argument ends with nothing resolved and both people feeling worse than when it started. What Is Actually Happening: Both partners entered the argument already at elevated emotional arousal. The flooding in one partner triggered shutdown in the other. Without regulation skills, neither person was able to access the prefrontal capacity needed for problem-solving or empathy. The argument was not really about the dishes. |
| The Situation: A couple has an argument that begins over something small: who was supposed to do the dishes. |
| Scenario 4: A Good Day That Ends Badly |
| What It Looks Like From Outside: The good feeling disappears immediately. The person becomes irritable, then despairing. They cannot access the positive feelings from hours earlier. What Is Actually Happening: People with emotional dysregulation often have difficulty carrying emotional states forward across time. A positive emotion does not protect against a negative trigger the way it might in people with more robust regulation. The baseline is also more variable, meaning the floor can drop quickly. |
| The Situation: The person has had a genuinely good day and is feeling relaxed and positive. Then a minor inconvenience occurs, like being stuck in traffic. |
Signs of Emotional Dysregulation — A Self-Reflection Guide
The following questions are designed to help you reflect on whether emotional dysregulation is a significant feature of your experience. They are not a diagnostic tool. They are a structured reflection aid.
| Do you experience this regularly? | Sometimes | Often / Always |
| My emotional reactions feel more intense than other people’s in the same situation | Yes | |
| I go from calm to overwhelmed very quickly, sometimes without understanding why | Yes | |
| After getting upset, it takes me a long time to calm down and return to normal | Yes | |
| I say or do things when I am upset that I later regret and would not have done when calm | Yes | |
| Small frustrations or inconveniences can ruin my entire day | Yes | |
| I sometimes feel nothing — completely numb or shut down — when I should be feeling something | Yes | |
| I have been told I am too sensitive or that I overreact | Yes | |
| My emotions feel physical: heart racing, tightness in chest or stomach, difficulty breathing when upset | Yes | |
| I avoid certain situations because I am afraid of the emotional reactions they might produce | Yes | |
| My mood changes significantly and quickly, sometimes multiple times per day | Yes | |
| When I feel rejected or criticized, even mildly, the emotional pain is intense | Yes | |
| I use substances, food, social media, or other things to manage or escape from difficult emotions | Yes |
If you answered Often or Always to four or more of these items, emotional dysregulation is likely playing a significant role in your daily experience and is worth addressing with professional support. If you answered Often or Always to seven or more, the impact is likely substantial and professional evaluation is strongly recommended.
Conditions Associated with Emotional Dysregulation
Emotional dysregulation is a transdiagnostic feature: it appears across many different clinical conditions rather than being specific to one. Understanding which conditions most prominently involve emotional dysregulation helps clarify why the same core issue can look so different across presentations.
Borderline Personality Disorder
BPD is defined by emotional dysregulation as its central feature. The biosocial theory was developed specifically to explain BPD’s development. Every one of the nine DSM-5 criteria for BPD either directly describes emotional dysregulation or is a consequence of it: fear of abandonment, unstable relationships, identity disturbance, impulsivity, self-harm, mood instability, chronic emptiness, explosive anger, and dissociation. DBT was developed by Marsha Linehan specifically to treat BPD and remains its most evidence-supported treatment.
PTSD and Complex PTSD
Trauma fundamentally disrupts emotional regulation systems. The hypervigilance of PTSD represents a chronically activated threat-detection system. The emotional flooding episodes, the sudden overwhelm, the alternating numbness and intensity, are all expressions of a nervous system that was reorganized by overwhelming experience. Complex PTSD, which develops from repeated relational trauma, involves particularly severe and pervasive emotional dysregulation.
ADHD
Emotional dysregulation in ADHD is increasingly recognized as a core feature, not a peripheral symptom. Rejection-sensitive dysphoria, the intense emotional pain triggered by perceived criticism or rejection, is particularly prominent and particularly undertreated. ADHD medication addresses attention and impulsivity but often does not fully address the emotional dysregulation dimension, which is why DBT skills are increasingly being incorporated into ADHD treatment.
Depression and Anxiety
Both depression and anxiety involve significant emotional dysregulation, though the presentation differs. Depression often involves difficulty accessing positive emotions alongside intense negative emotional states. Anxiety involves a chronically activated threat-detection system that amplifies and sustains anxious emotion beyond what the situation warrants. Emotional dysregulation both contributes to these conditions and is maintained by them.
Autism Spectrum Disorder
Many autistic individuals experience significant emotional dysregulation, though for reasons that partially differ from other presentations. Difficulties with interoceptive awareness, meaning sensing one’s own physical and emotional states, sensory sensitivities that amplify emotional responses, and the cumulative stress of navigating a neurotypical world all contribute. Emotional dysregulation in autism requires approaches that account for these specific factors.
Emotional Dysregulation and Relationships
Emotional dysregulation does not stay inside the person who experiences it. It reverberates through every significant relationship in their life, and the relational consequences are often what finally bring someone to seek help.
The Pattern From the Outside
People in relationships with someone who has significant emotional dysregulation often describe a particular experience: the sense that they are constantly walking on eggshells, unable to predict which response a given action or statement will produce. They may have learned to avoid certain topics, to monitor their partner’s or family member’s emotional state before speaking, and to feel responsible for preventing or managing emotional episodes.
This relational dynamic is painful for both parties. The person with emotional dysregulation typically does not want their reactions to affect others the way they do. The pattern is driven by the emotional system, not by intent. But unaddressed, it can progressively erode the trust and intimacy in even the most committed relationships.
Rejection-Sensitive Dysphoria and Relationships
Rejection-sensitive dysphoria describes the intense emotional pain, often described as physically painful, that is triggered by perceived criticism, rejection, or failure. For people who experience RSD, a partner’s neutral tone, a slightly critical comment, or even an unanswered message can produce a pain response that feels catastrophic.
The behavioral consequences of RSD are significant: people may become intensely defensive, may withdraw to protect themselves from perceived rejection, may make accusations or demands that seem entirely disproportionate to the partner, or may suppress their own needs to the point of resentment in order to avoid triggering what they fear will be rejection.
DBT Skills Specifically for Emotional Dysregulation
DBT was built from the ground up to address emotional dysregulation. Its four skill modules each target different aspects of the problem. The following skills are the most directly relevant to the core dimensions of emotional dysregulation.
| Mindfulness Module — Observe and Describe |
| Why It Helps: Emotional dysregulation is partly maintained by the inability to identify what is being felt. Observation creates a moment of space between the emotion and the behavioral response. You cannot regulate what you cannot name. Practical First Step: When you notice you are upset, pause and ask: what is this? Is it anger, fear, shame, hurt, or something else? Name it without judgment. Even partial naming reduces the emotion’s unprocessed intensity. |
| Mindfulness Module — Wise Mind |
| Why It Helps: Wise Mind is the integration of emotional experience and rational thought. It counters the tendency to make decisions from pure emotion mind when flooded. Accessing Wise Mind creates space for values-based responding rather than emotion-driven reacting. Practical First Step: When in a high-distress state, ask: what would my Wise Mind say about this? If you cannot access it, the first step is to reduce the emotional intensity using distress tolerance skills before attempting Wise Mind. |
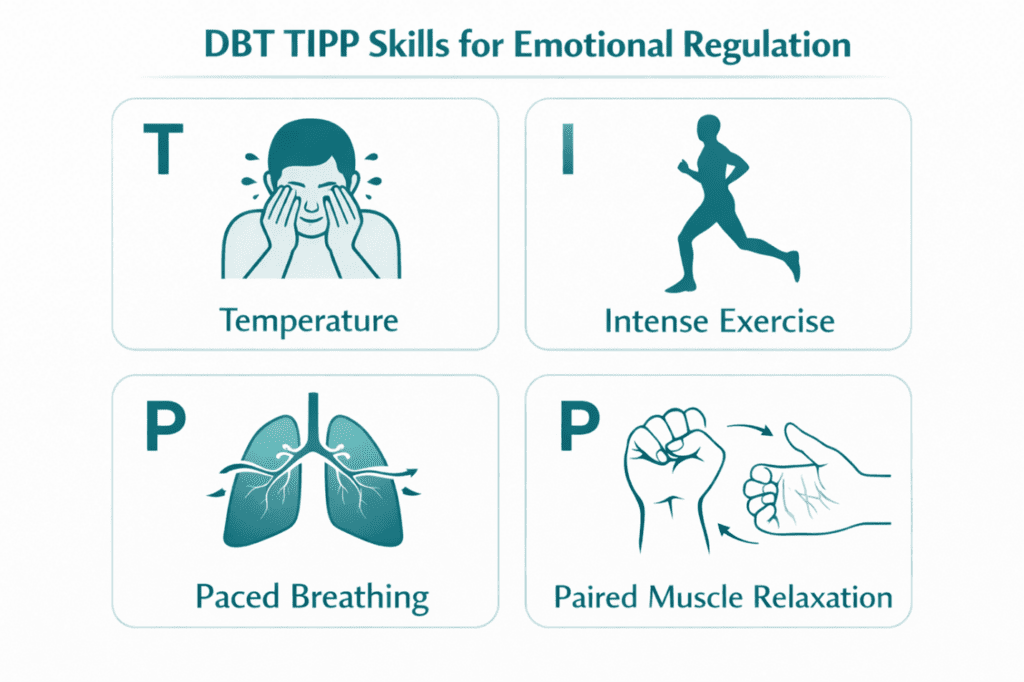
| Distress Tolerance Module — TIPP Skills |
| Why It Helps: TIPP (Temperature, Intense exercise, Paced breathing, Progressive relaxation) targets the physiological arousal that underlies flooding. Because emotional dysregulation is partly a bodily state, directly intervening in the physiology can bring intensity down faster than cognitive strategies alone. Practical First Step: At the first sign of flooding, try paced breathing: inhale for 4 counts, exhale for 6. The longer exhale activates the parasympathetic system. Alternatively, hold ice cubes or splash cold water on your face to trigger the dive reflex. |
| Distress Tolerance Module — Radical Acceptance |
| Why It Helps: Much of the suffering in emotional dysregulation comes from the secondary layer: fighting against the emotion, demanding it not be present, resisting what is already happening. Radical acceptance reduces this secondary suffering by accepting the emotional reality without requiring it to be different. Practical First Step: Notice when you are resisting an emotional state: I should not feel this way, this is stupid, make it stop. Instead, try: I am feeling this. It makes sense that I am feeling this. I do not have to agree with it or act on it. This acceptance does not make the emotion stronger; it often reduces its intensity. |
| Emotion Regulation Module — Check the Facts |
| Why It Helps: Emotional dysregulation often involves emotional responses that are more intense than the facts of the situation warrant. Check the Facts examines whether the emotion fits the actual situation or whether the intensity is coming from interpretation, past experience, or threat-pattern activation. Practical First Step: Ask: what are the actual facts? What am I adding to the facts in my interpretation? If a friend did not text back, the facts are: no text. The interpretation that they are angry or done with you is not a fact. Separating facts from interpretation reduces emotional intensity. |
| Emotion Regulation Module — Opposite Action |
| Why It Helps: Emotions drive action urges: shame urges withdrawal, anger urges attack, fear urges escape. When the action urge is not justified or will make things worse, doing the opposite disrupts the emotion-behavior cycle and can actually change the emotion itself. Practical First Step: Identify the action urge your emotion is producing. Ask whether acting on it will help or worsen the situation. If worsening: do the opposite. If shame urges you to hide, make eye contact and hold your head up. This does not suppress the emotion. It changes its trajectory. |
| Interpersonal Effectiveness Module — DEAR MAN |
| Why It Helps: Much emotional dysregulation occurs in interpersonal contexts. DEAR MAN (Describe, Express, Assert, Reinforce, Mindful, Appear confident, Negotiate) provides a structure for communicating needs and setting limits even when emotional intensity is high, reducing the reactivity that unstructured conflict produces. Practical First Step: Before a potentially difficult conversation, plan what you want to say using DEAR MAN. Describe the situation factually. Express your feeling. Assert what you need. Having a structure reduces the chance that the conversation triggers flooding. |
Treatment for Emotional Dysregulation
Emotional dysregulation is treatable. The evidence base is strongest for treatments that directly target the regulatory mechanisms rather than only the symptoms or conditions that emotional dysregulation produces.
Dialectical Behavior Therapy (DBT)
DBT is the most evidence-supported treatment specifically designed to address emotional dysregulation. It is the first-line treatment for BPD and has strong evidence for PTSD, depression, eating disorders, and presentations involving self-harm and suicidality, all of which involve significant emotional dysregulation as a central feature.
Comprehensive DBT delivers four skill modules (covered in Part 9), individual therapy that addresses diary-card-tracked behaviors using a treatment hierarchy, phone coaching for between-session support, and therapist consultation to ensure treatment quality. The combination of these components produces outcomes that no single component produces alone.
The DBT-Linehan Board of Certification is the highest available standard for verifying that a therapist is delivering comprehensive, adherent DBT. This certification matters because diluted or informal DBT produces significantly weaker outcomes, particularly for severe emotional dysregulation.
CBT and ACT
Cognitive Behavioral Therapy addresses emotional dysregulation through the cognitive dimension: identifying and restructuring the interpretive patterns that amplify emotional responses. It is effective for milder presentations and for specific anxiety and depressive conditions where emotional dysregulation is a secondary feature.
Acceptance and Commitment Therapy, which shares significant overlap with DBT’s acceptance-based components, focuses on building psychological flexibility and values-based action rather than symptom reduction. It is particularly useful for emotional dysregulation associated with avoidance and experiential avoidance patterns.
Medication
No medication directly treats emotional dysregulation as a standalone diagnosis. Medications may help by treating underlying conditions that contribute to dysregulation. Mood stabilizers may reduce emotional lability. SSRIs may reduce the baseline anxiety that amplifies emotional reactivity. Non-stimulant medications for ADHD may address the rejection-sensitive dysphoria dimension. Medication is typically most useful as an adjunct to therapy rather than as a primary treatment.
What Recovery from Emotional Dysregulation Looks Like
Recovery from emotional dysregulation does not mean becoming emotionally flat or never having intense feelings. It means developing enough regulatory capacity that intense feelings no longer drive your life in directions you do not want to go.
People who have worked through significant emotional dysregulation typically describe a gradual change in the relationship to their emotional experience rather than a single transformation. The amygdala still fires. The emotional sensitivity that came from their biology is still present. What changes is the space between feeling and acting, the window of tolerance that widens with practice, and the access to skills that make intense emotion survivable without it being destructive.
Many people who have been through this process describe their emotional sensitivity, once it is regulated, as a genuine strength: a capacity for depth of experience, empathy, and connection that people without that sensitivity do not have access to in the same way. The goal of treatment was never to make them less feeling. It was to make the feelings theirs to work with rather than forces that worked against them.
| From Our Clients | I have learned to feel emotions that I thought were impossible to feel. I can communicate more effectively. I am learning to face tough situations without giving up. In the last three years I have experienced tremendous growth. I am forever grateful. |
Getting Support
If what you have read in this guide resonates with your experience, the most important next step is reaching out to a mental health professional with specific training in emotional dysregulation and DBT.
Emotional dysregulation is not a character flaw. It is not something you are doing wrong. It is a pattern that developed for reasons that were not your fault, in a nervous system that was responding the only way it knew how. And it is one of the most treatable presentations in mental health when approached with the right tools and the right relationship.
| Struggling with Emotional Dysregulation? Southside DBT specializes in comprehensive, board-certified DBT treatment for emotional dysregulation, BPD, PTSD, anxiety, and co-occurring conditions via telehealth across Georgia. Kelly Pinnick | DBT-Linehan Board of Certification, Certified Clinician (770) 880-2538 | kelly@southsidedbt.com Accepting: Aetna | Anthem BCBS GA | Cigna | United Healthcare | Self-Pay $150/session |
